It's 7:48 AM on a Monday. The phones at a mid-sized primary care practice are already ringing. By the time the first medical assistant sits down with a headset, there are nine calls in queue. One is a diabetic patient trying to refill insulin. Another is a new mother who's been on hold for twelve minutes, trying to schedule her six-week postpartum visit. A third is a Spanish-speaking patient who will eventually hang up because there's no one available who speaks his language.
By 10 AM, a third of those callers will have abandoned the line entirely. Some will try again tomorrow. Some will go to urgent care. Some will simply go without care.
This isn't a worst-case scenario. For thousands of practices and health systems across the country, this is just Monday.
A Crisis Hiding in Plain Sight
The healthcare industry talks a lot about innovation, AI-powered diagnostics, precision medicine, virtual care. But behind those headlines, the most fundamental part of the patient experience remains stubbornly broken: getting through the front door.
80% of patient access still happens by phone. And half of those calls go unanswered. Not because staff don't care, but because there simply aren't enough of them to keep up. The math doesn't work anymore.
On the clinical side, providers are spending upward of 15.5 hours every week on EHR documentation, time that could be spent with patients. On the administrative side, provider teams are managing upwards of 25 refills per day, per clinician. The work is tedious, repetitive, and relentless.
The toll on patients is measurable. Average scheduling backlogs have stretched to 31 days. Nearly half of all patients report frustration with long hold times, poor communication, and the exhausting experience of having to repeat their information every time they call. They aren't angry at their doctor. They're exhausted by the system around their doctor.
And the toll on the business is just as real. 43% of self-scheduled appointments happen after hours, times when most practices are completely dark. Every one of those missed interactions is lost revenue, a lost quality touchpoint, and a lost opportunity to keep patients engaged. For organizations tied to value-based care, the stakes are enormous. Medicare Advantage quality bonuses alone represent a $12.7 billion pool, and access and experience metrics are among the biggest levers that determine who earns those dollars.
This is not a problem that another round of hiring can fix. Turnover in healthcare administration is at historic highs. Recruiting is expensive. Training takes months. And even fully staffed teams can't be everywhere at once, across every channel, every language, every hour of the day.
The system needs something fundamentally different.
Enter Agentic AI: The Technology That Changes the Equation
Over the past several years, AI in healthcare has largely meant one of two things: predictive analytics running quietly in the background, or rigid chatbots that could handle a narrow set of scripted interactions before dead-ending into "please call the office for further assistance."
Neither of those is sufficient for the complexity of real patient access.
But agentic AI is changing what's possible. Unlike traditional automation, which follows fixed rules, or conversational AI, which responds to prompts, agentic AI systems can reason, plan, and take autonomous action within defined boundaries. They don't just answer questions. They do work.
An agentic system can understand a patient's intent, evaluate clinical context, check real-time data, negotiate alternatives when a first option isn't available, and seamlessly escalate to a human when the situation demands it, all within a single interaction. It can maintain memory of who the patient is and what they've already said, across channels and over time. It can operate with empathy, adapt mid-conversation, and respect the guardrails that clinical and regulatory environments demand.
This is the inflection point. Not another chatbot bolted onto a website. Not another IVR tree that makes patients press buttons until they give up. Agentic AI represents a genuine digital workforce, one that can take on the high-volume, high-complexity tasks currently crushing administrative teams, while doing so with the contextual awareness and adaptability that patients actually need.
The technology is ready. The question for practices and health systems is no longer whether agentic AI can help. It's how fast they can put it to work in a scalable, compliant, and secure way.
Introducing XCaliber's AI-Powered Patient Navigator
This is exactly the problem XCaliber built to solve with our first AI Assistant.
Merlin is not a chatbot. It's a fully agentic AI Assistant and Digital Twin. Built on top of XCaliber's orchestration platform, the system of intelligence that connects to your EHR, understands your clinical and operational rules, and coordinates actions across every channel and workflow in real time. Where the platform is the engine, Merlin is the workforce it powers, designed to mirror the intuition, empathy, and problem-solving ability of a practice's best front-desk coordinator or care navigator.
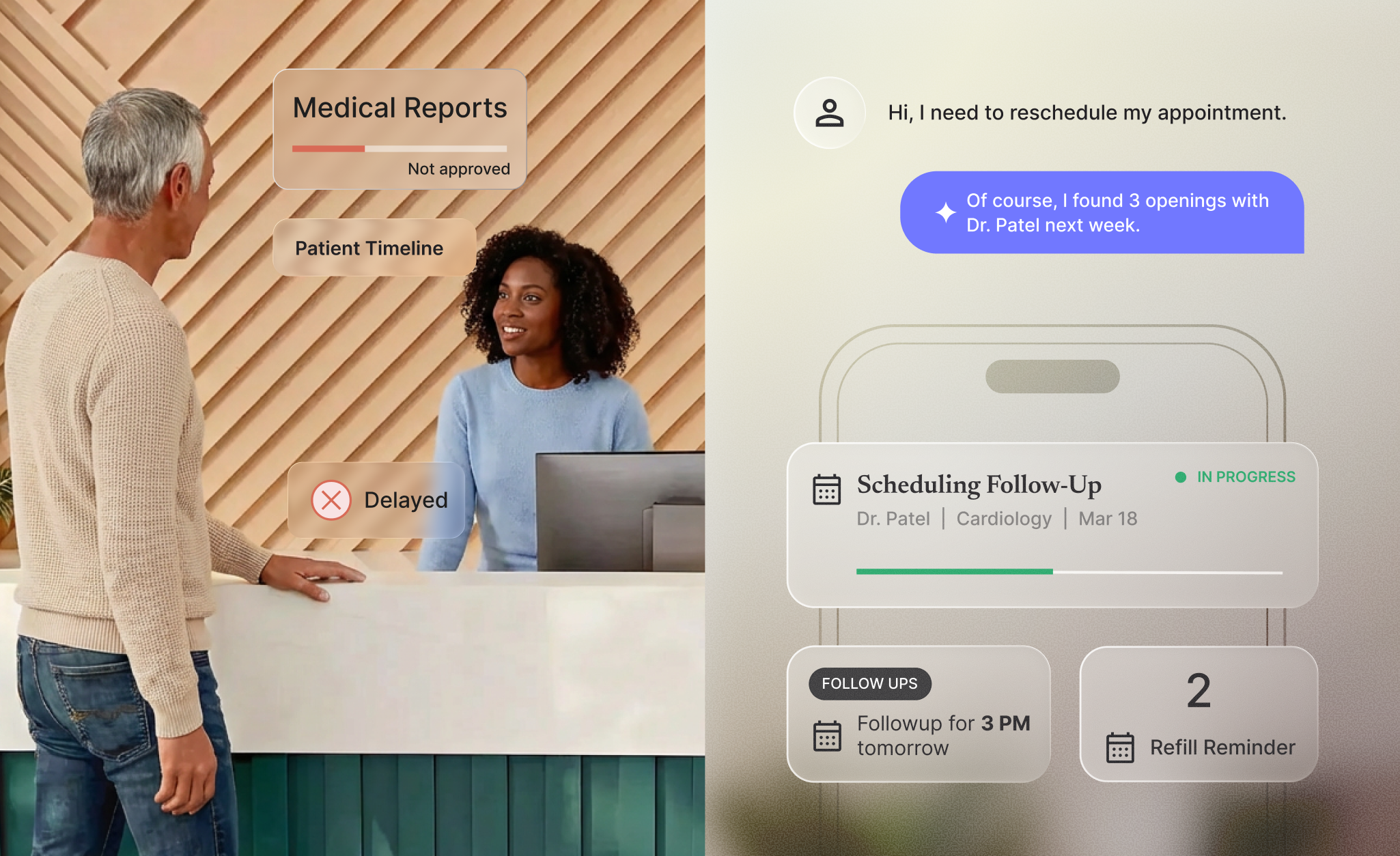
Think of the team member who knows every patient by name, never puts anyone on hold, speaks multiple languages fluently, and somehow navigates scheduling conflicts, prescription questions, and billing inquiries without missing a beat. Merlin is the digital twin of that person, operating at scale, across every channel, 24 hours a day.
Patients interact with Merlin the way they already communicate: by calling, texting, chatting on the web, or even sending a fax. No app to download. No portal to learn. No behavior change required. For staff, Merlin operates seamlessly within existing EHR workflows, no new platform to master, no six-month implementation to endure.
Intelligent Workflows That Go Far Beyond Scripted Automation
What makes the AI Patient Navigator genuinely agentic, and not just another automation layer, is its ability to handle complex, multi-step workflows that have historically required a trained human.
Scheduling with real negotiation. When a patient reaches out to book an appointment, XC’s Patient Navigator doesn't recite a list of open slots and call it done. It understands clinical urgency, reads real-time EHR availability, and if the patient's preferred time isn't open, it negotiates, offering alternative times, providers, or locations the way a skilled scheduler would. The interaction keeps moving forward instead of hitting a wall.
Waitlist recovery that turns cancellations into revenue. Every open slot is lost income. Patient Navigator actively monitors cancellations and proactively reaches out to waitlisted patients to fill them. Practices using this capability are recouping between $200,000 and $1.2 million annually, transforming a chronic revenue leak into a competitive advantage.
Prescription renewals with clinical intelligence and empathy. Patient Navigator evaluates refill eligibility against clinical rules, days' supply calculations, and medication restrictions. Routine renewals are processed automatically, eliminating up to 90% of manual refill work. For restricted medications, Patient Navigator doesn't simply reject the request. It explains clearly and compassionately why the renewal can't proceed, then escalates to the appropriate clinician with full context already attached, so no patient is left confused and no provider is left without the information they need.
Contextual memory that eliminates "Can you repeat that?" Patient Navigator maintains the thread of every patient interaction regardless of channel or timing. A patient who texts on Tuesday, calls on Wednesday, and chats online on Thursday never has to start over. And if they pivot mid-conversation, shifting from a scheduling question to a billing concern, Patient Navigator adapts seamlessly without forcing a transfer.
Multilingual support that expands access for every community. Language barriers are one of the most persistent equity gaps in healthcare. Patient Navigator provides fluent multilingual interaction without requiring practices to staff bilingual team members on every shift, ensuring that every patient receives the same quality of access regardless of the language they speak.
No Disruption. No App. No Lengthy Implementation. Just Results.
Operations and IT leaders have reason to be skeptical. Every new platform promises transformation and delivers a year-long implementation, a steep learning curve, and single-digit patient adoption. Merlin was designed to be the opposite of that experience.
XCaliber's implementation philosophy is deliberately lean: start with a focused use case, scheduling automation, after-hours access, chronic care support, integrate it securely within your existing environment, and test it in live production. Real-world data yields better insights in eight hours than months of closed simulation.
The results compound quickly. Practices running Merlin are automating 60 to 85% of inbound scheduling inquiries, reducing call abandonment by up to 88%, and cutting patient intake time from 15 minutes to 4. Administrative staff are reclaiming 5 to 40 or more hours per month, capacity redirected toward the complex, human-centered work that genuinely requires their expertise. Patient satisfaction holds at 9 out of 10. Repeat contacts drop by 50%. And 85% of after-hours interactions are resolved without any human intervention.
Built for Trust: Explainability, Control, and Compliance by Design
For clinical, IT, and risk leaders, the question is never just whether AI can do the work. It's whether you can trust it, and prove that trust to regulators, payers, and patients.
XCaliber built Merlin on three non-negotiable pillars: Explainability, Control, and Compliance.
Every action Merlin takes is observable and auditable. Engineers can trace the exact logic pathway and data inputs behind any decision, providing the transparency required for legal discovery, compliance reviews, and quality assurance. This is not a black box. It's a glass box with a complete paper trail.
Practice Managers retain full authority over Merlin's behavior. Its skills, escalation rules, and conversational personality are configurable to match the brand, tone, and clinical protocols of each individual practice. A pediatric clinic and a cardiology group don't operate the same way, and their AI assistant shouldn't sound the same either.
Clinical guardrails are embedded in the architecture, not bolted on after the fact. Merlin knows when to act, when to escalate, and when to step back. It is engineered to support clinical decision-making, never to replace it.
The Access Crisis Won't Wait. Neither Should You.
The challenges facing practices and health systems today aren't going to resolve themselves. You can't hire fast enough, train fast enough, or stretch your current team far enough to close the gap. But the technology to change the equation is here, and it's no longer theoretical.
Merlin represents a new operating model: one where your practice scales its capacity without scaling its headcount, where patients get immediate answers instead of hold music, and where your team finally has room to focus on the work that drew them to healthcare in the first place.
Ready to see what an agentic digital workforce can do for your practice? Schedule a demo and experience the future of patient navigation, live, in your environment, on your terms.